Understanding Modern Treatments for Degenerative Joint Conditions
- Vaibhav Sharma

- Mar 20
- 4 min read

Degenerative joint conditions affect millions of people and often develop gradually as cartilage and surrounding tissues wear down over time. These conditions can lead to persistent pain, stiffness, swelling, and reduced mobility that affect everyday movement.
Among them, knee osteoarthritis is a common cause of long-term joint discomfort, especially among older adults and those with previous knee injuries. It develops when cartilage in the knee gradually breaks down, causing inflammation and pain during everyday activities. In certain cases, specialists may recommend treatments such as genicular artery embolization for knee osteoarthritis.
In this article, we’ll explore modern treatments that help manage degenerative joint conditions and improve long-term mobility.
What Are Degenerative Joint Conditions?

Degenerative joint conditions gradually damage cartilage, bones, and surrounding tissues, causing persistent pain, stiffness, inflammation, and reduced joint mobility over time. Osteoarthritis is the most common form, often affecting the knees, hips, and hands. These conditions typically develop over time due to aging, joint overuse, injury, or genetic factors.
According to The Conversation, research shows that even young, active individuals are increasingly diagnosed with osteoarthritis earlier than expected. Globally, more than 600 million people live with this degenerative joint condition. Major risk factors include ageing, obesity, metabolic disorders, chronic inflammation, prior joint injuries, and repetitive mechanical stress on joints.
Non-Surgical Treatments That Help Manage Symptoms
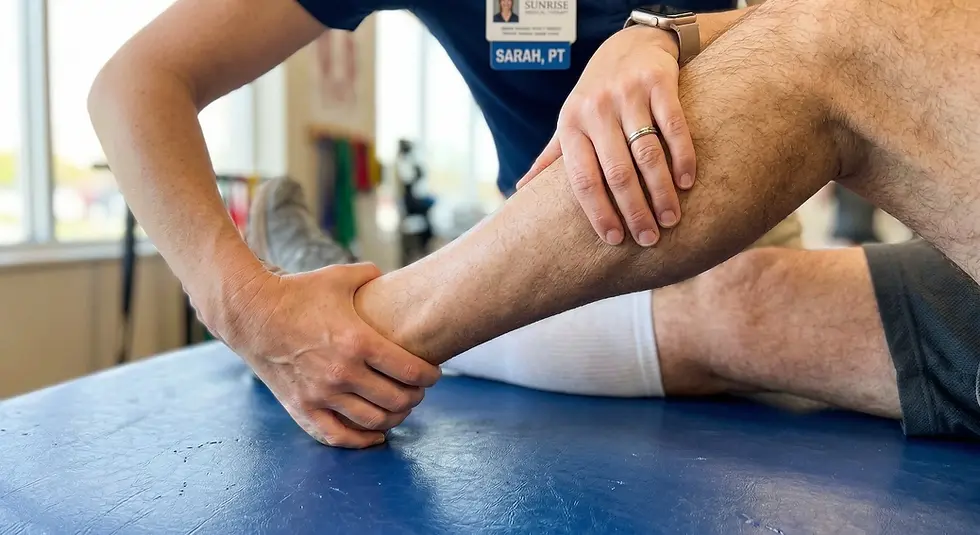
Non-surgical treatments aim to reduce pain, improve joint function, and slow the progression of degenerative joint conditions. Common approaches include physical therapy, low-impact exercises, weight management, pain-relief medications, and corticosteroid or hyaluronic acid injections. Orthotics and braces offer essential support to improve overall joint stability.
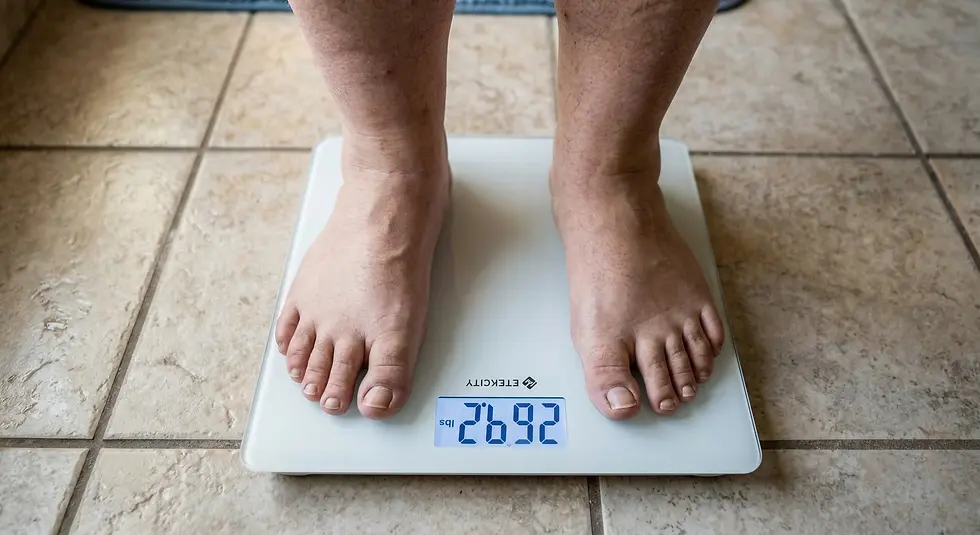
Weight management is a critical non-surgical intervention for joint preservation. Research published in Cureus highlights that excess body weight significantly accelerates mechanical degeneration. Specifically, data suggests that every 5 kg increase in weight raises the risk of knee osteoarthritis by 36%. Reducing this load is essential for long-term joint stability.
Emerging Minimally Invasive Treatment Options

Progress in medical technology has created minimally invasive options that serve as alternatives to conventional joint surgery. Doctors may recommend these procedures when conservative treatments fail to deliver sufficient relief. Specialists may recommend them for patients with persistent pain, reduced mobility, or inflammation despite therapy, medications, or injections.
One notable example is genicular artery embolization (GAE) for knee osteoarthritis, which targets specific blood vessels around the knee to reduce inflammation and pain. This minimally invasive approach avoids major surgery. It offers shorter recovery times, minimal tissue damage, and a faster return to daily activities.
Pedes Orange County notes that GAE is a minimally invasive procedure that avoids large incisions or stitches. This lowers complication risks and supports faster recovery. Because it is less invasive than surgery, most patients resume normal activities within days, often without extended hospital stays.
The Role of Regenerative and Injection-Based Therapies
Regenerative and injection-based therapies are gaining attention for managing degenerative joint conditions. Therapies such as Platelet-Rich Plasma (PRP), stem cells, and hyaluronic acid injections effectively mitigate inflammation while promoting biological tissue restoration. These minimally invasive options aim to restore joint function, relieve pain, and potentially slow the progression of joint degeneration.
The surge in clinical adoption is mirrored by a booming global market for these biological interventions. The Business Research Company reports that the regenerative joint therapy market reached $3.04 billion in 2025. Projections indicate growth to $5.88 billion by 2030, reflecting a robust 14.2% compound annual growth rate.
Surgical Solutions for Severe Joint Damage
Surgical intervention becomes necessary when joint damage progresses to a severe stage. Advanced osteoarthritis often necessitates joint replacement, corrective osteotomy procedures, or arthroscopy. These treatments effectively restore mobility and provide lasting pain relief.
Surgeons recommend these interventions when non-surgical and minimally invasive options fail. Modern techniques prioritize precision and reduced recovery times for optimal results. These advancements ensure long-term durability, helping patients effectively regain their independence and quality of life.
The National Institute of Health predicts a massive surge in surgical interventions by 2030. Total knee arthroplasty rates in the US are projected to rise by 673%. Similarly, total hip arthroplasties are expected to increase by 174%. This highlights the critical role of modern surgical solutions.
Choosing the Right Treatment Plan for Long-Term Joint Health
Choosing the right treatment plan for degenerative joint conditions requires a personalized and comprehensive approach. Doctors assess joint damage severity, age, lifestyle, and overall health before recommending therapies. Treatment plans may include physical therapy, medications, lifestyle changes, regenerative injections, or minimally invasive procedures based on patient needs.
Regular monitoring also helps physicians adjust treatments as conditions progress or symptoms change. Proactive treatment and ongoing management preserve joint health and future movement. Patients who actively participate in treatment decisions and follow recommended care often achieve better pain relief, improved joint function, and quality of life.
Frequently Asked Questions
At what age do degenerative joint conditions usually begin?
Degenerative joint conditions, such as osteoarthritis, typically begin in middle age, around 40 to 50 years old. Early onset can occur due to genetics, joint injuries, or repetitive stress. Risk increases with age, and by 65, nearly half of adults show some degree of joint degeneration.
How does physical activity influence joint degeneration?
Physical activity plays a dual role in joint health. Moderate, low-impact exercises like swimming, cycling, or walking strengthen muscles, support joints, and improve flexibility. However, repetitive high-impact activities or poor technique can increase cartilage wear and raise the risk of osteoarthritis.
How do doctors determine the severity of joint damage?
Doctors assess joint damage through physical examinations, medical history, and tests like MRI, X-rays, or CT scans. These evaluations reveal cartilage loss, bone changes, and inflammation. The findings help specialists determine degeneration severity and guide appropriate treatment plans.
Advancing Joint Health Through Informed Care

Modern treatments for degenerative joint conditions continue to evolve, offering patients more effective ways to manage pain and maintain mobility. From lifestyle modifications and non-surgical therapies to regenerative treatments and advanced surgical procedures, a wide range of options now exist.
Prompt detection and early treatment are essential for slowing the progression of joint disease. Personalized treatment plans developed with medical specialists help ensure the best possible outcomes. Combining medical care, healthy habits, and regular monitoring helps individuals protect joint health, improve mobility, and maintain an active lifestyle.









Comments